| |
Oral Anticoagulants and Antiplatelet Drugs
|
 |
Preface
|
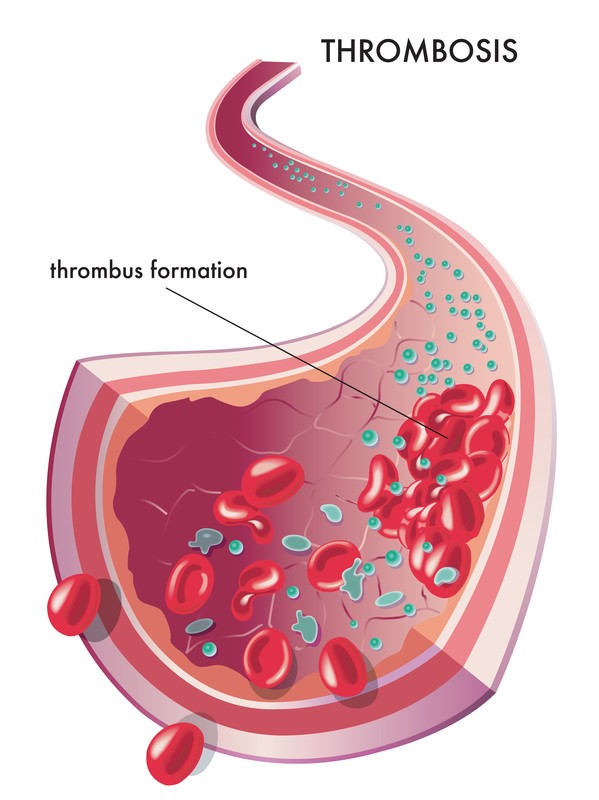
Blood clotting, or coagulation, is an important process that prevents excessive bleeding when a blood vessel is injured. Platelets and protein (clotting factors) in your plasma work together to stop the bleeding by forming a clot over the wound. Sometimes, however, clots form on the inside of vessels without an obvious injury or do not dissolve naturally. These situations can be dangerous and require accurate diagnosis and appropriate treatment including the use of a blood thinner.
|
If you have some kinds of heart or blood vessel disease, or if you have poor blood flow to your brain, your doctor may recommend that you take a blood thinner. Blood thinners reduce the risk of heart attack and stroke by reducing the formation of blood clots in your arteries and veins. You may also take a blood thinner if you have an abnormal heart rhythm called atrial fibrillation, heart valve disease, or congenital heart defects. |
|
|
▲ back to top
Treatment with blood thinners |
There are two types of blood thinners – anticoagulants and antiplatelet drugs. Anticoagulants work by interfering with blood protein to lengthen the time it takes to form a blood clot. Antiplatelet drugs prevent blood cells called platelets from clumping together to form a clot. Both types of drugs are effective in keeping a clot from forming or stopping the growth of a clot.
All registered anticoagulants in Hong Kong are prescription-only medicines and should be administered strictly under doctor’s instruction and recommendation. Some are available in oral dosage forms such as tablets and capsules, while others are only available in injectable forms. There are four oral anticoagulants available in Hong Kong, including the traditional drug warfarin, and the newer drugs dabigatran etexilate, apixaban, and rivaroxaban.
|
 |
Anticoagulants are considered more aggressive drugs than antiplatelet drugs. They are recommended primarily for people with a high risk of stroke and people with atrial fibrillation (a heart condition that causes a irregular heart rate). Other people with blood that clots easily, such as those who have deep vein thrombosis (blood clots in the deep veins of the legs) or pulmonary embolism (a blood clot in the lungs), may also benefit from anticoagulant therapy.
All registered antiplatelet drugs in Hong Kong are prescription-only medicines except aspirin. Some are available in oral dosage forms such as tablets and capsules, while others are only available in injectable forms. Low-dose aspirin is the most commonly used antiplatelet drug. Examples of other oral antiplatelet drugs include clopidogrel, ticlopidine, dipyridamole, prasugrel, and ticagrelor.
Low-dose aspirin is highly recommended for preventing a first stroke, but it and other antiplatelet drugs also have an important role in preventing recurrent strokes. Antiplatelet drugs may also be given if you have had acute coronary syndrome (heart attack or unstable angina) or a coronary stent.
|
|
|
▲ back to top
Classification of blood thinners |
Anticoagulants and antiplatelet drugs can be classified according to their mechanism of action.
Anticoagulants
Anticoagulants interfere with various clotting factors in the coagulation process to slow down the process. Oral anticoagulants can be classified as follows:
| 1. | Vitamin K antagonists: Inhibit the activation of the vitamin K-dependent clotting factors. The degree of depression of clotting factors is dose-dependent. The only vitamin K antagonist available in Hong Kong is warfarin. |
| |
|
 |
| 2. | Direct thrombin inhibitors (DTIs): Bind with thrombin which is the central effector of coagulation to inactivate thrombin. Example includes dabigatran etexilate.
|
| |
| 3. | Direct factor Xa inhibitors: Bind to clotting factor Xa specifically to block its activity. Examples include apixaban and rivaroxaban. |
Antiplatelet Drugs
Antiplatelet drugs describe agents which decrease platelet aggregation and inhibit thrombus (clot) formation. Platelet activation process involves the production of several platelet activation agonists including thrombin, thromboxane A2 (TXA2) and adenosine diphosphate (ADP), which amplify the platelet response and stimulate platelet aggregation. Oral antiplatelet drugs can be classified as follows:
| 1. | COX-1 inhibitor: Potent antiplatelet which inhibits platelet cyclooxygenase (COX), a key enzyme in the generation of TXA2 which is responsible for platelet activation and aggregation. The main member of this class is aspirin. |
| |
| 2. | P2Y12 receptor antagonists
| a) | Thienopyridine: Act by inhibiting the ADP-dependent pathway of platelet activation. Examples include ticlopidine, clopidogrel and prasugrel. |
| b) | Adenosine triphosphate analogue: Reversibly interact with the P2Y12 receptor to inhibit the receptor to prevent ADP-induced platelet aggregation. Example includes ticagrelor. |
|
| |
| 3. | Phosphodiesterase inhibitors: Inhibit adenosine uptake and cyclic GMP phosphodiesterase activity, thus decreases platelet aggregability. Phosphodiesterase inhibitor alone has little antiplatelet effect and is currently used in combination with other drugs. Example includes dipyridamole. |
|
|
|
▲ back to top
Common side effects and precautions
Drug class
|
Common side effects
|
Precautions
|
| Anticoagulants |
| 1. Vitamin K antagonist |
- haemorrhage
- nausea and vomiting
- diarrhea
- jaundice
- hepatic dysfunction
- pancreatitis
- pyrexia
- alopecia
- rash
|
- Use with caution in mild to moderate renal impairment. Monitor INR more frequently in severe impairment
- Not recommended for patients with severe hepatic impairment, or in first trimester of pregnancy
- Regular blood test to check how long it takes for your blood to clot (INR test) and dose may need to be adjusted
|
| 2. Direct thrombin inhibitors |
- haemorrhage
- nausea
- dyspepsia
- diarrhoea
- abdominal pain
- anaemia
|
- Use with caution in the elderly and in patients with low body weight
- Use with caution in patients with bleeding disorders, thrombocytopenia, recent biopsy or major trauma, oesophagitis, gastritis and oesophageal reflux
- Use with caution in patients taking concomitant drugs that increase risk of bleeding
- Not recommended for patients with active bleeding, or at significant risk of major bleeding, or with severe hepatic and renal impairment
- Not recommended in pregnancy or breastfeeding
|
| 3. Direct factor Xa inhibitors |
| |
Apixaban |
| |
- haemorrhage
- nausea
- bruising
- anaemia
|
| |
Rivaroxaban |
| |
- haemorrhage
- nausea and vomiting
- diarrhoea
- constipation
- dyspepsia
- abdominal pain
- dizziness
- headache
|
|
- Use with caution in patients at risk of bleeding, or taking concomitant drugs that increase risk of bleeding
- Not recommended for patients with active bleeding, or at significant risk of major bleeding, or with severe renal or hepatic impairment
- Not recommended in pregnancy or breastfeeding
|
| Antiplatelet Drugs |
| 4. COX-1 inhibitor |
- bronchospasm
- gastro-intestinal irriation such as nausea
- gastro-intestinal haemorrhage
- other haemorrhage (e.g. subconjunctival)
|
- Use with caution in patients with renal impairment, and during third trimester of pregnancy
- Use with caution in patients with asthma, uncontrolled hypertension, previous peptic ulceration, concomitant use of drugs that increase risk of bleeding, G6PD deficiency, dehydration and elderly patients
- Not recommended for patients with severe hepatic or renal impairment, with active peptic ulceration, haemophilia and other bleeding disorders, or with previous history of hypersensitivity to aspirin or other non-steroidal anti-inflammatory drugs (NSAID)
- Not recommended in breastfeeding
|
| 5. P2Y12 receptor antagonists |
| (i) Thienopyridine |
- haemorrhage
- rash
- gastrointestinal disturbances, such as dyspepsia, abdominal pain, diarrhea (common for ticlopidine and more frequent for geriatric patients)
- blood dyscrasia (most common for ticlopidine)
|
- Use with caution in patients with renal or hepatic impairment; avoid use in those with severe hepatic impairment
- Use with caution in patients at increased risk of bleeding, or with concomitant use of drugs that increase risk of bleeding
- Not recommended for patients with active bleeding
- Not recommended in pregnancy and breastfeeding
- Regular blood test for ticlopidine therapy for signs of blood dyscrasia
|
| (ii) | Adenosine triphosphate analogue |
|
- haemorrhage
- dyspnoea
- bruising
|
- Use with caution in patients at increased risk of bleeding, or with concomitant use of drugs that increase risk of bleeding, with cardiac conduction problem, asthma, chronic obstructive pulmonary disease
- Not recommended for patients with active bleeding or history of intracranial haemorrhage
- Not recommended in pregnancy or breastfeeding
- Monitor renal function 1 month after initiation
|
| 6. | Phosphodiesterase inhibitors |
|
- gastrointestinal effects
- dizziness
- myalgia
- throbbing headache
- hypotension
- severe bronchospasm and angioedema
- rash
- increased bleeding during or after surgery
|
- Use with caution in rapid worsening of angina, aortic stenosis, recent myocardial infarction, heart failure
- Use with caution in patients with concomitant use of drugs that increase risk of bleeding
- Use with caution in pregnancy or breastfeeding
|
|
|
▲ back to top
General advice
|
- Take warfarin once a day at the same time each day as prescribed, usually in the evening.
- If you accidentally miss a dose of warfarin, never take a double dose to catch up (unless specifically advised by a doctor).
- If you forgot to take your dose of antiplatelet drug, take the dose as soon as you remember, then continue to take your course as normal. Never double dose to make up for a missed dose.
- Take antiplatelet drugs with or after food to help reduce irritation to the stomach.
-
When you are taking warfarin,
-
Avoid binge drinking or getting drunk as doing this can increase the effect of warfarin and so increase the risk of bleeding.
- Maximum daily limit is three units of alcohol a day for man and two units a day for woman. One unit is roughly equivalent to half a pint of beer or a single measure (25ml) of a spirit such as vodka.
- Avoid situations that increase your risk of injury (e.g. sports that involve physical contact with other people).
- Seek immediate medical attention if you are bleeding a lot or it takes a long time for bleeding to stop.
- Get medical help if you have a hard blow to the head as you may have bleeding inside without knowing it.
|
|
|
|
▲ back to top
Communication with your doctor
|
|
- When you start taking warfarin as prescribed, tell your doctor about any medications or supplements that you are taking. Lots of herbal medicines and supplements can interact with warfarin. Do not start taking any new herbal medicines or supplements without checking with your doctor. Examples of such herbal medicines and supplements include dong quai, glucosamine, ginkgo biloba, ginseng, St. John’s wort, evening primrose oil, etc.
- If you receive new prescriptions from someone other than your usual medical provider, make sure you remind him that you are taking an anticoagulant or antiplatelet drug as the drugs may interact with each other.
|
 |
- Consult your doctor before making any major changes to your diet. Some foods contain large amounts of vitamin K and can interact with the effect of warfarin if eaten in large amounts. Examples include liver, green leafy vegetables such as broccoli and spinach, cranberry juice, garlic, black licorice and soybean.
- Tell your healthcare provider you are taking warfarin before you have any medical or dental procedures. Warfarin should usually be stopped 5 days before elective surgery.
- Seek advice promptly if you become pregnant or are planning a pregnancy as warfarin can be harmful to a baby, especially in the first trimester of pregnancy; aspirin increases the risk of bleeding during the third trimester of pregnancy; and some drugs should be altogether avoided in pregnancy.
- Tell your doctor if you are breastfeeding as some antiplatelet drugs are not recommended for use in breastfeeding women.
- Inform your doctor of your medical history as special precautionary measures may be warranted if you have certain diseases.
- Watch out for any unusual and serious side effects that develop. If you experience any such symptoms, contact your doctor immediately.
- Communicate with your doctor for the best treatment option. Your doctor will prescribe the most appropriate drugs for you after considering your condition and your response to the drugs.
|
|
▲ back to top
Storage of anticoagulants and antiplatelet drugs
Anticoagulants and antiplatelet drugs should be kept in a cool and dry place. Unless specified on the label, medicines should not be stored in refrigerators. Furthermore, drugs should be kept properly in places unreachable by children to prevent accidental ingestion.
|
|
▲ back to top
|
|
Acknowledgement: The Drug Office would like to thank the Professional Development and Quality Assurance (PD&QA) for their valuable contribution to the preparation of this article.
|
|
|
|
|